Measles was eliminated in the United States in 2000, and for years most parents never had to think about it. Now, it is back.
As of April 2026, there have been over 1,700 confirmed cases across the country, including Texas, with most linked to ongoing outbreaks.¹ The measles resurgence we are seeing today is largely happening in communities where declining vaccination rates have left gaps in protection, making it easier for the virus to spread.
If your child is unvaccinated or you are unsure about their vaccination status, it is important to stay informed.
What’s Actually Causing the Measles Resurgence?
The virus didn’t change. What changed is how protected we are against it.
Measles spreads through the air. One infected person can pass it to up to 18 unvaccinated people in the same space. The virus can hang in the air for two hours after someone leaves a room. That level of contagion means even a small gap in community immunity is enough to start an outbreak.
And right now, the gaps are growing.
Declining vaccination rates are the most direct cause of this measles resurgence. The MMR vaccine is highly effective, but only when enough people receive it. Communities need strong, widespread vaccination coverage to keep measles from spreading. Many areas are now falling short, creating the conditions for outbreaks to return.
Why are fewer kids getting vaccinated?
- Misinformation, especially the long-debunked autism claim has pushed some parents away from the MMR vaccine
- COVID-19 disrupted routine childhood vaccination schedules globally, leaving millions of kids behind on their shots
- Limited access to healthcare in certain areas means appointments get missed and never rescheduled
- International travel is reintroducing the virus from countries where measles never went away
When these factors come together, measles finds an opening to spread again. Without timely action, even a single imported case can move quickly through an under-vaccinated classroom or community and turn into a larger outbreak.
Measles Doesn’t Start With a Rash
This is where many parents get caught off guard.
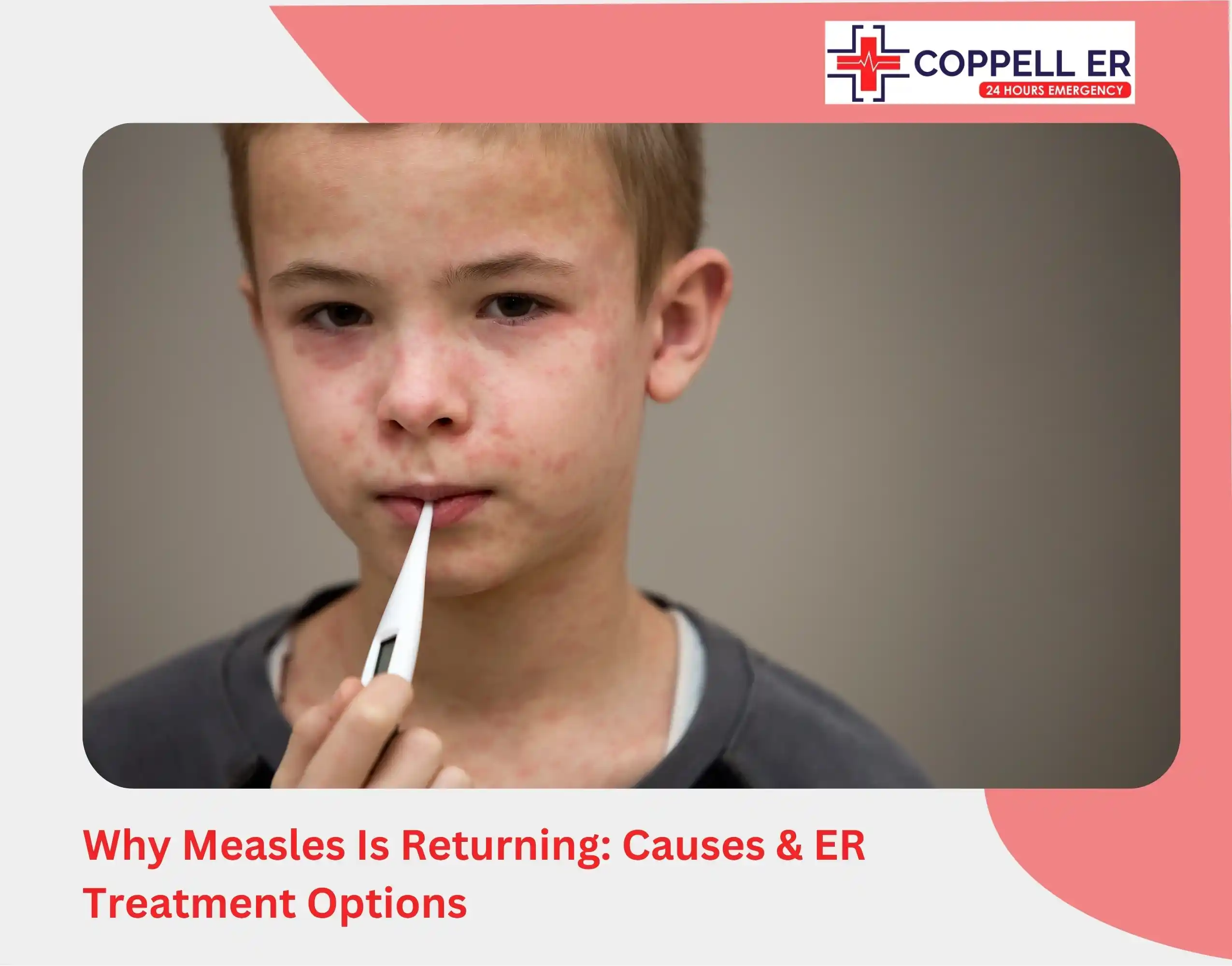
By the time the rash shows up, your child has already been spreading the virus for several days. Early on, measles doesn’t stand out; it looks like a typical cold or flu, with high fever, a runny nose, a persistent cough, and red, watery eyes. A few days later, tiny white spots can appear inside the cheeks, one of the first clues that this isn’t just another routine illness.
Then the rash begins at the face and gradually moves downward, spreading across the neck, chest, arms, and legs over the next few days.
During a measles resurgence, it is important to look beyond symptoms alone. Think about recent exposure your child may have had, whether they were around someone who was sick, traveled recently, or spent time in crowded settings. These details can be just as important as the symptoms themselves when it comes to identifying measles early.
The Complications Are What Make Measles Dangerous
Measles is not just a rash and a fever that passes. The real danger is what comes after, and measles complications can escalate quickly.
Here’s what can happen:
- Pneumonia, which is one of the most serious complications and a leading cause of measles-related deaths in children
- Ear infections that can lead to permanent hearing loss
- Encephalitis (brain swelling), which can cause seizures, brain damage, or even death
- A rare but fatal brain disease called SSPE that can appear years after recovery, with no cure
There’s also a lesser-known complication called immune amnesia. Measles can weaken the immune system by erasing parts of its memory, making your child more vulnerable to other infections long after the initial illness. The impact goes far beyond the rash and fever.
Measles complications do not always appear while the rash is active. Some develop after your child seems to be getting better. That is why close monitoring matters, and why knowing when to go to the ER is so important.
When to Go to the ER
Not every measles case needs emergency care. But some do, and things can change quickly.
Go to the ER right away if you notice:
- Breathing that is fast, labored, or includes wheezing
- A high fever that does not come down with medication
- Signs of dehydration, like a dry mouth, no tears, or not urinating for several hours
- Extreme drowsiness or trouble waking your child
- Seizures or a sudden change in behavior
- Symptoms that seem to improve and then suddenly get worse
That last pattern matters. A short period of improvement followed by a sudden decline can signal a serious complication. Do not let one good day create a false sense of relief.
If something feels off, trust that instinct and act. Getting care earlier gives medical teams more time and more options to help.
What ER Treatment for Measles Looks Like
There is no medication that can eliminate measles once it starts. ER treatment focuses on supporting the body, managing symptoms, and stepping in early to prevent complications from becoming life-threatening.
When a patient arrives with measles, the first step is isolation. Measles is airborne and highly contagious, so protecting other patients and staff is immediate.
From there, ER treatment for measles typically includes:
- Oxygen support if breathing is affected
- IV fluids to treat dehydration
- Vitamin A supplementation, proven to reduce measles severity and lower the risk of death in children
- Fever management and continuous monitoring
- Antibiotics if a secondary bacterial infection like pneumonia has developed
- Neurological monitoring if encephalitis is suspected
Children need closer monitoring because their condition can shift quickly. In pediatric cases, ER treatment for measles may include lab testing, imaging, and observation services when needed to catch complications early.
For those who have been exposed but are not yet showing symptoms, there are still time-sensitive options. The MMR vaccine may help prevent infection if given soon after exposure. Immune globulin, a protective antibody treatment, can also be used within a short window for infants and others at higher risk.
How Declining Vaccination Rates Keep Outbreaks Going
Once measles gets into a community with low vaccination coverage, it moves quickly. One infected person exposes a classroom. That classroom carries it home. Families then bring it into everyday spaces like events, games, and gatherings.
Declining vaccination rates do not just affect unvaccinated children. They also take away protection from infants who are too young to be vaccinated, from immunocompromised children who cannot receive the vaccine, and from people whose immunity has weakened over time.
That is why a measles resurgence is a community issue, not just an individual one. The more gaps in protection, the easier it is for the virus to keep spreading.
What You Should Do Right Now
Check your child’s vaccination records. Two doses of the MMR vaccine are needed for full protection. If they are behind, contact your pediatrician and schedule catch-up vaccination as soon as possible.
If you suspect your child has been exposed to measles, call ahead before visiting a clinic or ER. This allows healthcare teams to prepare isolation measures and helps protect other patients in the waiting area.
Stay updated on local outbreaks. During a measles resurgence, public health departments track and report cases. Knowing whether measles is circulating in your area can help you better interpret early symptoms.
Key Takeaway
Measles has returned because declining vaccination rates created the conditions it needs to spread. The measles resurgence we are seeing now is closely tied to communities that no longer have enough protection to keep the virus contained.
Know the symptoms and stay alert to measles complications that can still develop even after the rash begins to fade. If breathing becomes difficult, a high fever will not come down, or something feels seriously wrong, do not wait. Go directly to the ER. ER treatment for measles cannot cure the infection, but it can prevent severe outcomes and save lives.
Do not wait for a second warning sign. Walk in anytime or call us at 469-763-3136.
FAQs
1. How long is measles contagious?
Measles is highly contagious from about 4 days before the rash appears to 4 days after it shows up. This long contagious window is one reason outbreaks spread quickly, especially in areas with declining vaccination rates. Even brief exposure in shared spaces like schools or waiting rooms can lead to transmission.
2. What kills the measles virus?
There is no specific medicine that instantly kills the measles virus once infection begins. The body clears it over time with supportive care, which is why prevention through vaccination is so important during a measles resurgence. If symptoms become severe, ER treatment measles focuses on managing fever, dehydration, and breathing issues rather than directly killing the virus.
3. What food to avoid for measles?
There are no strict food restrictions for measles, but it helps to avoid foods that are hard to digest or can worsen discomfort when dealing with measles complications like sore throat, nausea, or diarrhea.
4. What age is measles most serious?
Measles tends to be most serious in children under 5, adults over 20, pregnant individuals, and anyone with weakened immunity. Severe measles complications like pneumonia or brain inflammation are more likely in these high-risk groups.
5. What is the difference between measles and rubella?
Measles is a highly contagious virus that often causes high fever, cough, red eyes, and a spreading rash, and it can lead to serious complications like pneumonia or brain inflammation. Rubella is usually milder, with low fever and rash, but it can be dangerous in pregnancy.