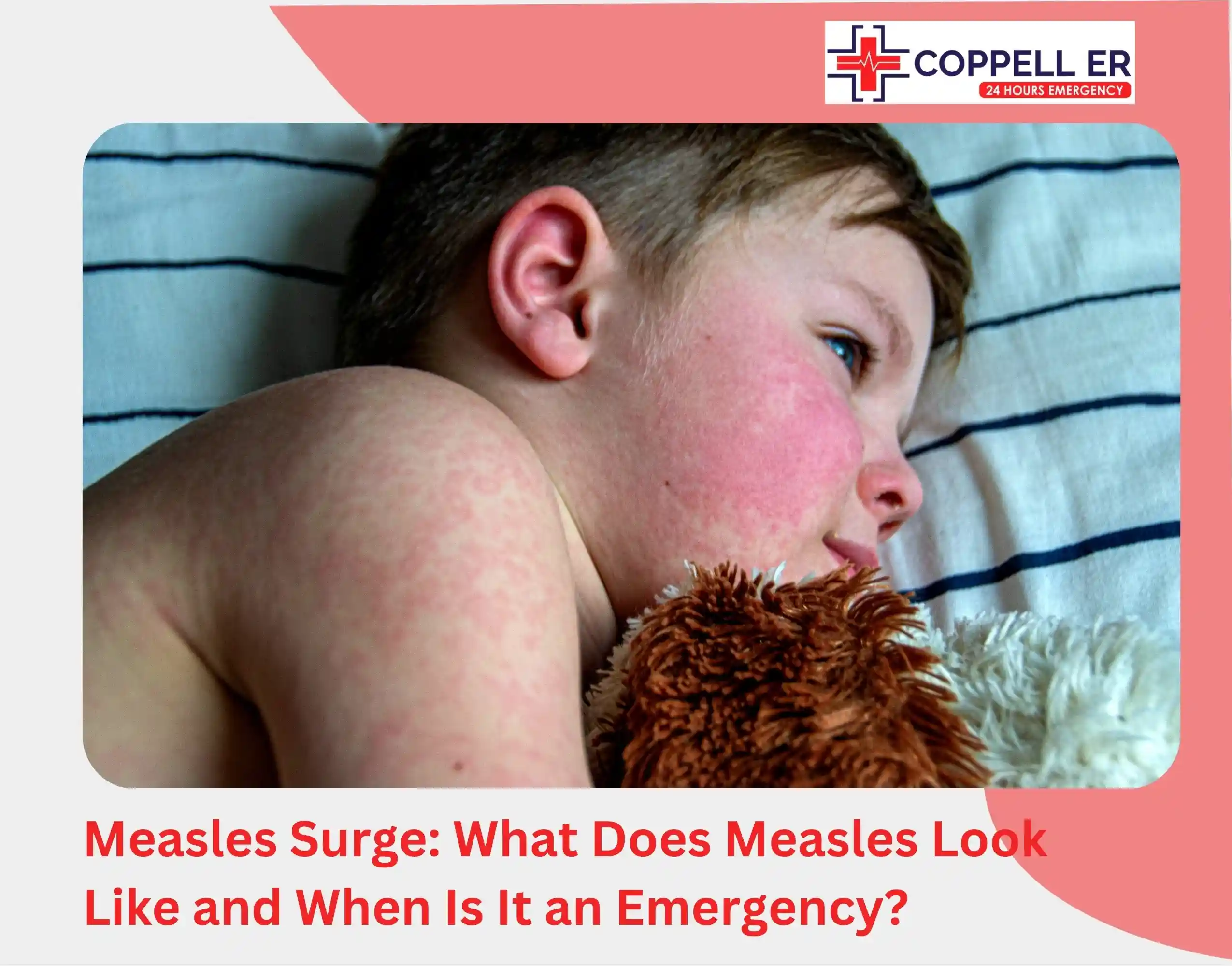
What Does Measles Look Like? Measles symptoms do not start with a rash. They start with a high fever, harsh cough, and bloodshot eyes that look a lot like a bad cold, and by the time the rash shows up days later, your child has already been contagious for four days.
With measles outbreaks still surfacing in undervaccinated communities, recognizing early measles symptoms is the fastest way to protect your household and get ahead of complications before they escalate.
What Is Measles?
Measles (rubeola) is a viral infection that spreads through respiratory droplets when an infected person coughs, sneezes, or even talks. What separates it from other childhood infections is sheer contagiousness: up to 90% of unvaccinated people in close contact with an infected person will catch it. The virus can linger in the air for up to two hours after the infected person has left the room.
Before widespread vaccination began in 1963, measles infected millions of children annually in the U.S. alone. Cases dropped dramatically after that, but periodic measles outbreaks in undervaccinated communities prove this childhood infection has not disappeared.
Early Measles Symptoms: The First Warning Signs
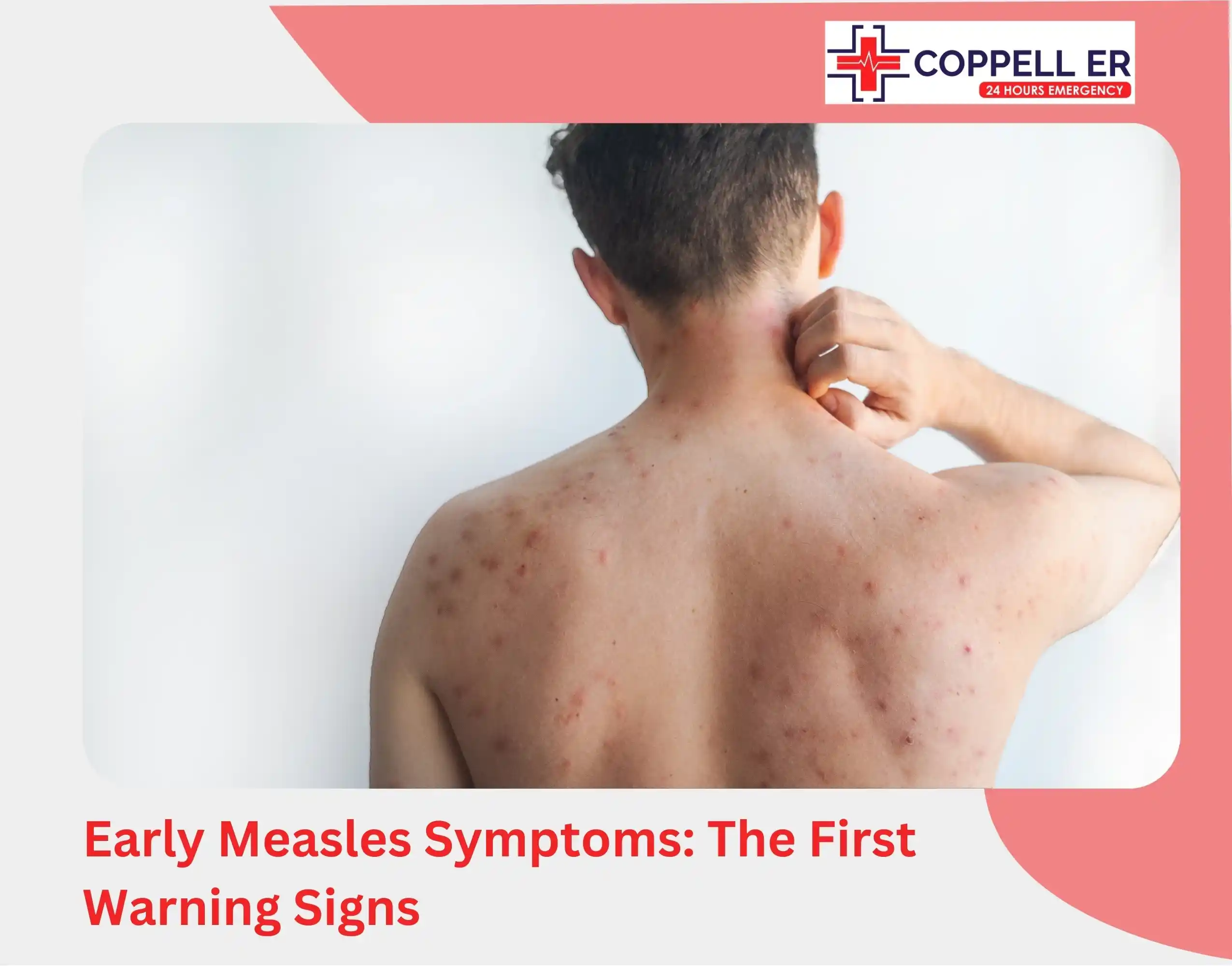
The rash gets all the attention, but it is actually a late sign. Initial measles symptoms appear 10 to 14 days after exposure and look almost identical to a cold or flu, which is exactly why so many cases go unrecognized in the early window.
This prodromal stage lasts two to four days before the rash appears:
- High fever — often the first sign, frequently spiking to 104°F or higher. It may dip briefly, then climb even higher once the measles rash
- Persistent dry cough — harsh and worsening, sometimes severe enough to cause breathing difficulties in younger children.
- Runny nose and congestion — indistinguishable from a cold at this stage, which is why most parents do not suspect measles yet.
- Red, watery eyes (conjunctivitis) — bloodshot, light-sensitive, and distinctly worse than typical cold-related eye irritation. Doctors refer to cough, runny nose, and conjunctivitis as the “3 C’s” of measles.
- Koplik’s spots — tiny white spots with bluish-white centers on the inner cheeks, opposite the molars. These are unique to measles and can confirm a diagnosis before the rash ever appears. They fade once the rash emerges.
The Measles Rash
The measles rash is the hallmark most people picture, but it does not show up until several days after other measles symptoms have already taken hold. Knowing what it looks like, and how it differs from rashes caused by other infections, helps narrow the diagnosis fast.
The rash typically emerges three to five days after initial symptoms begin, starting as flat red spots on the face along the hairline and behind the ears. Over the next few days, it spreads downward across the neck, trunk, arms, legs, and feet. As it progresses, the spots may merge together, creating larger patches of red, bumpy skin.
The measles rash blanches (fades temporarily) when pressed, a useful way to distinguish it from rashes that do not. It typically lasts five to six days, then fades in the same top-down order it appeared, sometimes leaving behind a brownish discoloration or light peeling.
Fever often spikes again during the rash phase, sometimes reaching dangerous levels. This is when patients feel worst and when complications like pneumonia are most likely to develop.
How a Measles Outbreak Spreads
A measles outbreak typically begins with a single case; often a traveler returning from a region where measles circulates widely. From there, the virus moves fast. One infected person in an airport terminal, grocery store, or medical waiting room can expose hundreds of people, and the virus remains airborne for up to two hours after that person has left.
Public health officials respond aggressively to every measles outbreak because community spread can accelerate within days, especially in areas where vaccination rates have dipped below the threshold needed for herd immunity.
Measles Complications: Why This Childhood Infection Is Dangerous
Most children recover from measles without lasting damage. But this childhood infection carries a complication rate that surprises many parents, particularly for children under five, adults over 20, pregnant women, and anyone with a compromised immune system.
A rare but devastating long-term complication called subacute sclerosing panencephalitis (SSPE) can develop seven to ten years after measles, causing progressive nervous system deterioration that is fatal in every case.
Complications like these are the reason measles vaccination exists, and why missing it carries real consequences.
When to Go to the ER for Measles

Most measles cases resolve at home with rest, fluids, and fever management. But certain measles symptoms cross into emergency territory. Knowing when to visit the ER for measles can prevent a manageable illness from becoming a life-threatening one.
Seek emergency care immediately if you or your child experiences:
- Labored breathing, wheezing, or rapid breathing may signal pneumonia or respiratory failure. If the skin takes on a bluish tint, call 911 or head to the ER for measles
- Severe headache combined with stiff neck, confusion, seizures, or loss of consciousness could signal encephalitis and requires immediate emergency evaluation.
- Persistent vomiting or severe diarrhea, especially with dehydration signs like reduced urination, dry mouth, or lethargy in children.
- Fever above 104°F unresponsive to medication, or any fever that persists beyond four days after the rash appears.
- Chest pain or worsening cough with breathing difficulty may indicate pneumonia developing and requires urgent assessment at an ER for measles-related respiratory issues.
Infants under one, pregnant women, and immunocompromised individuals should be monitored closely even if symptoms seem mild; these groups face the highest complication rates from measles.
Measles Symptoms by Age: What Looks Different in Babies, Kids, and Adults
- Infants and toddlers tend to deteriorate faster. They may refuse to eat or drink, leading to rapid dehydration, and their fevers can spike dangerously high before the rash even appears. Any infant with suspected measles warrants close medical supervision.
- School-aged children follow the classic progression; fever and cold-like symptoms first, followed by the measles rash three to five days later. This is the age group most commonly affected during a measles outbreak.
- Adults who contract measles often experience more intense symptoms than children: higher fevers, longer recovery, and a greater risk of pneumonia and hospitalization. Adults who were never vaccinated or received only one dose are the most vulnerable.
Measles Prevention and Protection

The MMR vaccine, covering measles, mumps, and rubella, remains the single most effective protection. Two doses provide roughly 97% immunity. Children typically receive dose one between 12 and 15 months and dose two between ages four and six.
If you are unsure about your vaccination status or your child’s, check with your healthcare provider. During an active measles outbreak, unvaccinated individuals should limit public exposure and ask about post-exposure vaccination or immune globulin, both of which can reduce severity if given within days of contact.
Key Takeaway
Measles follows a predictable arc, with fever and cold-like symptoms hitting first, followed by rash several days later. But complications can develop quickly in between. There is no antiviral treatment, so management is supportive: fluids, rest, and fever control at home.
The moment breathing becomes difficult, fever stops responding to medication, or your child becomes unusually lethargic, it is time for the ER.
If your child develops emergency measles symptoms, ER of Coppell is open 24/7 with on-site imaging, labs, oxygen therapy, and IV hydration. No appointment needed!
FAQs
1. What is considered an outbreak of measles?
A measles outbreak occurs when two or more related cases appear in a community or area, signaling active spread of the virus.
2. What are the symptoms of the breakthrough measles?
Breakthrough measles happens in vaccinated individuals and usually causes milder symptoms such as low-grade fever, mild rash, cough, and runny nose.
3. Why are parents refusing the measles vaccine?
Reasons vary and include concerns about vaccine safety, fear of side effects, religious or philosophical beliefs, and a general distrust of healthcare institutions. Public health agencies continue to address these concerns through transparent data and education.
4. What are the 3 C’s of the measles?
The 3 C’s include cough, coryza (runny nose), and conjunctivitis (red, watery eyes).
5. Is measles 100% curable?
No. There is no antiviral that targets measles directly. Treatment is supportive, including rest, fluids, fever management, and most people recover fully. Vaccination remains the only reliable way to prevent infection.