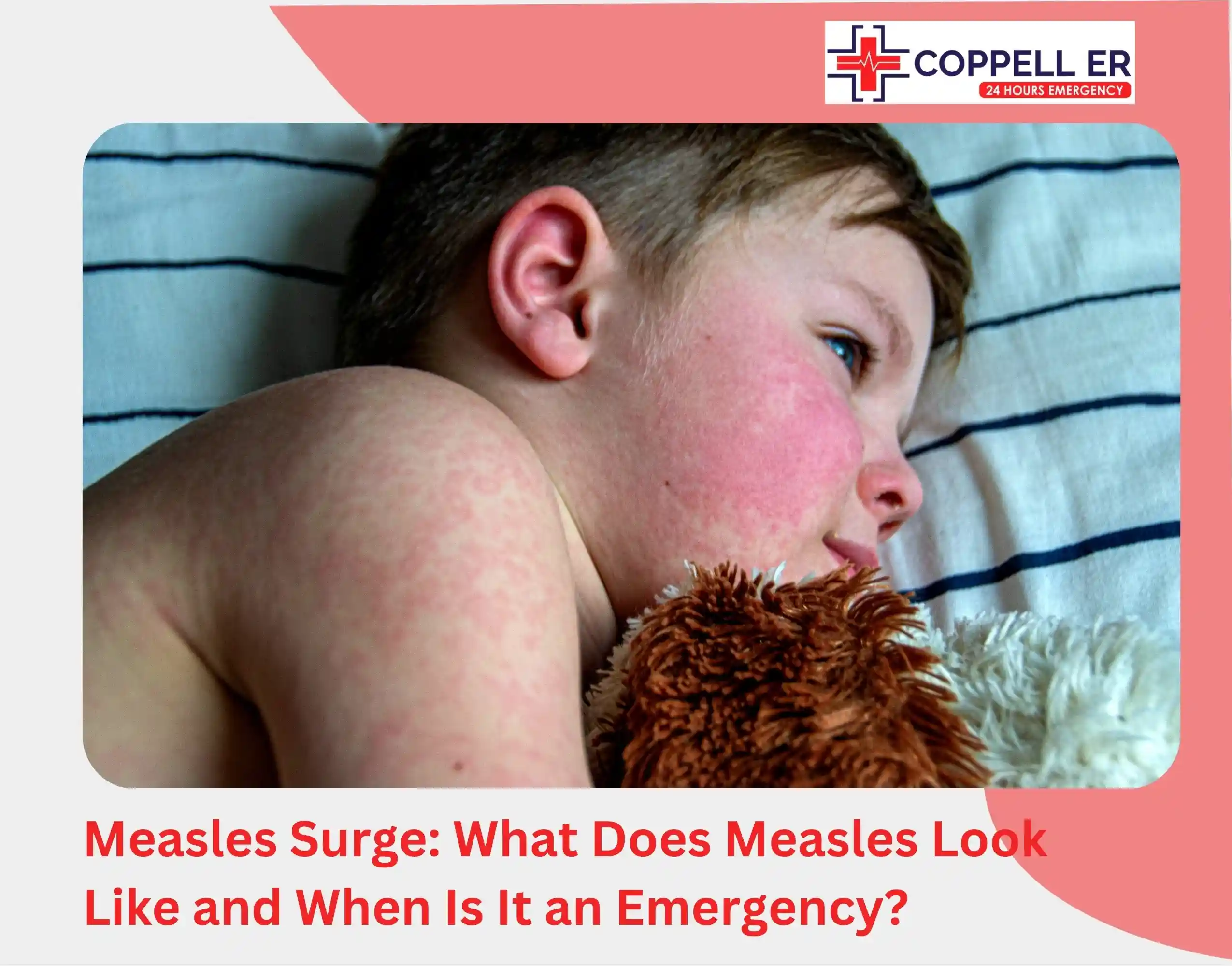
Every cold and cough season brings the same worry for parents: Is this the flu, COVID-19, or something else? With multiple respiratory viruses circulating at once, it’s easy to feel unsure about what you’re dealing with.
Let’s understand the differences between flu vs COVID vs RSV so that you can make confident decisions about your child’s health and know when it’s time to seek emergency care.
What Flu, COVID, and RSV Have in Common
All three are respiratory viruses that attack the airways and lungs. All three spread easily through close contact. And all three can escalate quickly in young children, older adults, and anyone with underlying health conditions.
That’s exactly what makes distinguishing between flu vs COVID vs RSV so difficult at home. The early respiratory infection symptoms often look identical: fever, cough, congestion, fatigue. But the trajectory of each virus, and who it hits hardest, is very different.
Knowing those differences could change your child’s outcome.
RSV: The One That Hits Kids the Hardest

RSV starts like a cold. That’s the problem.
In the first day or two, RSV symptoms in kids look harmless: a little congestion, a mild cough, maybe a low fever. Parents assume it will pass. Then it doesn’t.
Within 48 to 72 hours, things can shift fast. Breathing becomes harder. The cough gets worse. Infants stop feeding.
Watch for these RSV symptoms in kids closely:
- Wheezing or a high-pitched sound with each breath
- Rapid, labored breathing
- Nostrils flaring with effort
- Chest visibly sinking in with each inhale
- Bluish color around the lips or fingertips
- Unusual fatigue or difficulty staying awake
- Refusing to eat or drink
RSV is the leading cause of bronchiolitis and pneumonia in babies under 12 months. There is no standard antiviral treatment for most children. That means early recognition of RSV symptoms in kids is the only real defense.
If your child’s breathing changes in any way, don’t wait. Learn more about getting ahead of RSV quickly.
How Flu vs COVID vs RSV Actually Differ
Each virus has its own signature. When you’re comparing flu vs COVID vs RSV, onset and symptom pattern matter as much as the individual signs.
The Flu arrives fast and hard. One hour you’re fine. Next, you can’t get off the couch.
Key flu signs include:
- Sudden high fever, often 102°F to 104°F
- Severe muscle aches and chills
- Intense fatigue from the start
- Dry cough and sore throat
- Headache
- Vomiting or diarrhea, especially in children
Flu cases often spike in predictable waves. If you’re curious about seasonal patterns, check out our guide on the late-winter flu rebound.
COVID-19 has shifted with each variant, but respiratory infection symptoms remain central. It tends to build more gradually than the flu and can linger longer.
Distinct COVID signs include:
- Loss of taste or smell
- Prolonged fatigue lasting days or weeks
- Fever, body aches, and chills
- Cough and shortness of breath
- Sore throat and headache
- Nausea or diarrhea
RSV in adults often feels like a mild cold and resolves on its own. In young children, it is a completely different virus with a completely different risk level.
When comparing flu vs COVID vs RSV, think of it this way. The flu hits hard and fast. COVID builds and lingers. RSV looks mild until it isn’t, especially in infants.
Why Overlapping Symptoms Make Testing Critical

The frustrating reality is that all three viruses cause overlapping respiratory infection symptoms. Fever, cough, congestion, sore throat, and fatigue appear across all three viruses.
You cannot reliably tell them apart by symptoms alone.
At-home COVID tests give you a starting point, but flu and RSV testing requires a clinical visit. Getting tested matters because treatment decisions depend on the correct diagnosis. Tamiflu can reduce flu severity if given early. Antivirals are available for certain COVID cases. RSV, by contrast, is managed with supportive care, which means monitoring breathing closely and acting quickly if symptoms worsen.
Testing also protects others. Knowing which virus you’re carrying helps prevent spreading it to high-risk people in your home or community.
When to Go to the ER for Breathing Problems
This is the part that matters most.
Breathing difficulties during respiratory virus season are one of the most common reasons families visit the ER for breathing problems, and for good reason. Respiratory distress can go from concerning to critical in a matter of hours.
Go to the ER immediately if you see:
- Labored or rapid breathing that isn’t improving
- Nostrils flaring or the chest pulling inward with each breath
- Bluish or grayish color around the lips, face, or fingernails
- High fever in an infant under 3 months that is not responding to medication
- Extreme sleepiness, your child is hard to wake or unusually limp
- Signs of dehydration, no wet diapers in 8 hours, no tears, dry mouth
- Confusion or loss of consciousness in older children or adults
Don’t try to manage breathing problems at home. Arriving earlier gives medical teams more options and more time to act.
Adults with asthma, COPD, heart disease, or a weakened immune system should treat any worsening respiratory infection symptoms as an emergency. All three viruses can push an underlying condition past its threshold quickly. If you or your child has asthma, pay extra attention during virus season.
What Happens When You Arrive at Coppell ER
You won’t be left waiting when breathing is on the line.
Our emergency team begins assessment immediately. We test rapidly for flu vs COVID vs RSV so your care starts on the right path from the beginning.
Depending on the situation, treatment may include:
- Oxygen therapy and respiratory support
- Bronchodilators to open the airways
- IV fluids for dehydration and stabilization
- Antiviral medications when indicated
- Continuous monitoring throughout your stay
From infants in respiratory distress to adults struggling to breathe, we handle the full range of complications around the clock with no wait times. Our freestanding ER is equipped with on-site labs, CT scans, and pediatric care designed for exactly these situations.
Young children with respiratory illness also face a secondary concern: croup, which can develop alongside viral infections and narrow the airway further.
Key Takeaway
Flu vs COVID vs RSV share symptoms, but they are not the same virus, and they don’t carry the same risks for every patient.
Watch RSV symptoms in kids carefully, especially in the first year of life. Treat overlapping symptoms as a reason to test, not a reason to wait. And when breathing becomes labored, rapid, or visibly difficult, go straight to the ER for breathing problems.
Serious respiratory distress doesn’t come with a second warning. If something doesn’t feel right, trust that instinct. Walk in anytime, or call us at 469-763-3136.
[Get Directions to Coppell Emergency Room]
FAQs
1. What are the most dangerous respiratory infection symptoms?
Trouble breathing, chest pain, persistent high fever, confusion, and extreme fatigue are the most concerning signs. In children, look for rapid breathing, rib retractions, and refusal to eat or drink. Any breathing difficulty warrants an immediate ER visit.
2. Is RSV still going around?
Yes. RSV circulates year-round but peaks in fall and winter. It remains one of the most common causes of hospitalization in infants under 6 months. Parents should stay alert for wheezing, fast breathing, and feeding difficulties during virus season.
3. Is RSV more dangerous than COVID for children?
For infants and toddlers, RSV is typically the greater immediate threat. It’s the top cause of bronchiolitis and pneumonia in babies. COVID tends to cause milder illness in young children, though exceptions exist in kids with underlying conditions.
4. How long is someone contagious with RSV?
Most people are contagious for 3 to 8 days with RSV after symptoms begin. Young children may shed the virus longer, sometimes up to 4 weeks. RSV can spread before symptoms appear, which makes containment difficult in daycares and schools.
5. Can you have the flu and COVID at the same time?
Yes. Co-infection is rare but documented. Having both viruses simultaneously can increase the severity of illness, especially in older adults and people with chronic conditions. Testing for both helps guide treatment and monitoring.