Just when you think the flu season is almost over, people start getting sick again. After flu cases slow down in January, many emergency rooms see another rise in February and March. This is known as the Late-Winter Flu Rebound & Influenza B surge.
This flu second wave isn’t random. It usually happens because Influenza B becomes more active later in the season, even after Influenza A has already peaked.
Here is why the flu second wave happens, how Influenza B differs from what circulated earlier, and when symptoms require emergency flu care.
Why Does the Flu Come Back in Late Winter?
Flu season does not follow a single arc. The first wave, typically peaking between December and early January, consists primarily of Influenza A strains. These strains spread rapidly, cause severe symptoms, and dominate early-season headlines. As these cases decline, many people assume the worst is behind them.
That assumption proves dangerous. Influenza B strains, which circulate at lower levels during the initial surge, gain momentum as winter progresses. By late February and March, Influenza B often becomes the dominant circulating strain, creating what epidemiologists call a flu second wave.
Several factors drive this Late-Winter Flu Rebound & Influenza B pattern:
- Behavioral Changes: As Influenza A cases drop, people relax their guard. They stop washing hands as frequently, return to crowded indoor spaces, and abandon other protective behaviors that limited transmission earlier in the season.
- School Transmission: Children serve as primary vectors for Influenza B transmission. Unlike Influenza A, which affects all age groups severely, Influenza B particularly impacts school-aged children. When kids return from winter break and spend weeks in close quarters, transmission accelerates.
- Viral Competition: Influenza A and B strains compete for hosts. When Influenza A dominates the early season, Influenza B circulates at lower levels. As population immunity to Influenza A builds through infection and vaccination, Influenza B finds more susceptible hosts.
- Weather Patterns: Late winter conditions, cold temperatures combined with indoor crowding, create ideal transmission environments. The virus survives longer on surfaces and in air during these weeks.
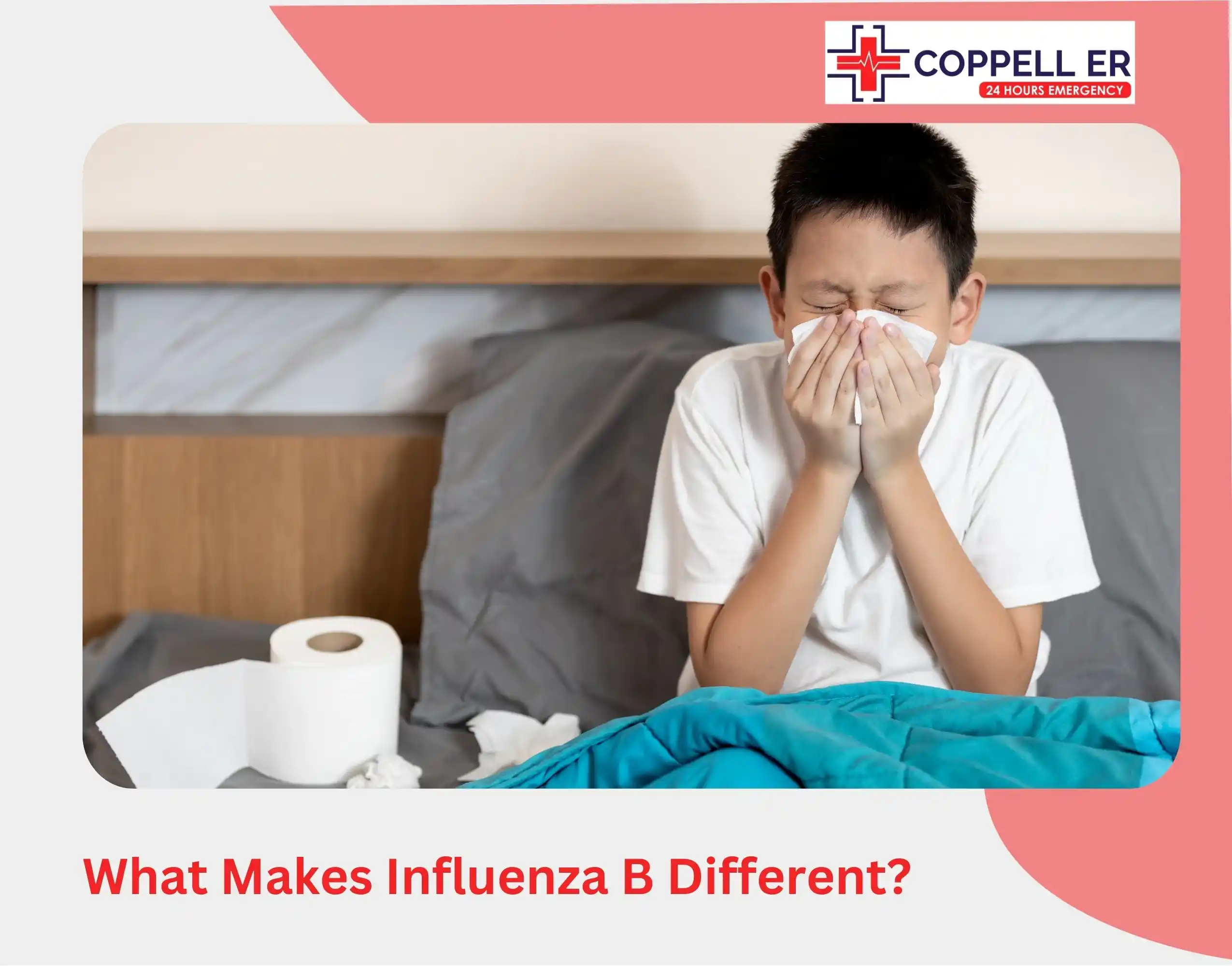
What Makes Influenza B Different?
The late-winter flu rebound & Influenza B catches people off guard because it does not behave quite like the Influenza A strain they may have already fought off.
Influenza B mutates more slowly than Influenza A, which means vaccine protection often remains more consistent against these strains. However, this slower mutation rate doesn’t make Influenza B less dangerous. It simply evolves on a slower timeline.
Symptoms of Influenza B often include:
- High fever lasting several days
- Severe muscle aches and body pain
- Extreme fatigue that persists for weeks
- Gastrointestinal symptoms, particularly in children (nausea, vomiting, diarrhea)
- Respiratory symptoms that may be milder initially but can worsen
Many people mistake Influenza B for a stomach bug during early stages, especially when gastrointestinal symptoms dominate. This confusion delays treatment and allows continued transmission to others.
The flu second wave driven by Influenza B tends to hit children and younger adults harder than elderly populations, though all age groups remain vulnerable. This demographic shift means the surge often goes underestimated until pediatric cases spike across emergency departments.
How Do You Know If You Have Influenza B?
Only a lab test can confirm whether you have Influenza B versus another respiratory virus or even a repeat Influenza A infection. Rapid diagnostic tests available at Coppell ER can identify the specific strain within minutes.
Key indicators suggesting Influenza B infection include:
- Sudden Onset: Symptoms appear abruptly, unlike the gradual progression of common colds. You feel fine one hour and severely ill the next.
- High Fever: Temperatures typically spike above 101°F (38.3°C) and may reach 104°F (40°C), particularly in children.
- Severe Fatigue: The exhaustion accompanying Influenza B exceeds normal tiredness. Many people describe being unable to get out of bed for days.
- Muscle Pain: Body aches affect multiple muscle groups simultaneously, causing significant discomfort that interferes with movement and sleep.
- Late-Season Timing: If you develop severe flu-like symptoms in February or March, particularly if you or your children already had flu earlier in the season, Influenza B becomes more likely.
When Does Influenza B Require Emergency Care?
Most Influenza B cases resolve with rest, hydration, and over-the-counter symptoms relief. But certain warning signs mean it’s time to head to the ER for flu care:
Emergency Warning Signs in Adults
Seek immediate emergency flu care if you experience:
- Difficulty Breathing or Shortness of Breath: When breathing becomes labored at rest or you cannot complete sentences without gasping, your lungs may be compromised by viral pneumonia or secondary bacterial infection.
- Persistent Chest Pain or Pressure: Influenza can trigger cardiac complications, particularly in people with underlying heart conditions. Chest discomfort accompanying flu symptoms requires immediate evaluation.
- Severe Dizziness or Confusion: Mental status changes indicate insufficient oxygen delivery to the brain or dangerous dehydration levels requiring IV fluid replacement.
- Persistent Vomiting: Inability to keep down fluids for more than 12 hours leads to dangerous dehydration, especially when combined with fever.
- Flu Symptoms That Improve Then Suddenly Worsen: This pattern often signals secondary bacterial pneumonia, a serious complication requiring antibiotics and potentially hospitalization.
Emergency Warning Signs in Children
Parents should bring children to the ER for flu treatment when they observe:
- Rapid or Difficult Breathing: Count your child’s breaths. Rates exceeding 60 per minute in infants, 40 per minute in toddlers, or 30 per minute in older children warrant emergency evaluation.
- Bluish Skin Color: Cyanosis around lips, fingernails, or face indicates insufficient oxygen levels requiring immediate intervention.
- Severe Irritability or Lethargy: Children who cannot be consoled or won’t wake up properly need urgent medical assessment.
- Seizures: Febrile seizures can occur with high fevers and require immediate medical attention.
- Symptoms of Dehydration: No tears when crying, significantly reduced urination, or extreme thirst indicate dangerous fluid loss.
Who Faces the Highest Risk During the Flue Second Wave?
The late-winter flu rebound and Influenza B surge hits certain groups harder:
- Young Children: Those under five years, particularly infants under two, experience more severe Influenza B illness and higher hospitalization rates.
- Pregnant Women: Pregnancy changes immune function and lung capacity, increasing vulnerability to severe influenza complications at any stage of gestation.
- Chronic Health Conditions: People with asthma, diabetes, heart disease, or compromised immune systems face elevated risks of influenza-related complications.
- Elderly Adults: While Influenza B affects this group less severely than Influenza A, those over 65 still face significant risks, particularly with underlying health conditions.
- Healthcare Workers: High exposure rates combined with long shifts and stress increase infection risk and severity.
What Happens During Emergency Flu Care?
If your flu symptoms bring you to the ER, here is what treatment typically involves:
- Antiviral Medications: Drugs like oseltamivir (Tamiflu) work best when started within 48 hours of symptom onset but can still provide benefits even when started later in severe cases.
- Oxygen Support: Patients with respiratory distress may require supplemental oxygen through nasal cannulas or masks to maintain adequate blood oxygen levels.
- IV Fluids: Dehydration from fever, vomiting, or inadequate oral intake requires intravenous fluid replacement to prevent organ damage.
- Antibiotics: While antibiotics don’t treat viral infections, they become necessary when secondary bacterial pneumonia develops.
- Respiratory Treatments: Nebulized medications can help open airways and improve breathing in patients with influenza-triggered asthma or bronchospasm.
How to Protect Your Family During Preventing the Late-Winter Flu Rebound & Influenza B Surge
Even if you were vaccinated earlier in the season, that protection still matters. Flu vaccines typically hold up well against Influenza B strains, though effectiveness varies year to year.
Additional prevention strategies include:
- Maintain Hygiene Practices: Continue frequent handwashing, even as case numbers from the first wave decline. The virus remains highly contagious during the second wave.
- Avoid Sick Contacts: When possible, maintain distance from people showing flu symptoms, particularly in late winter weeks.
- Disinfect High-Touch Surfaces: Doorknobs, light switches, phones, and keyboards harbor influenza virus particles that can remain infectious for hours.
- Monitor School Absenteeism: High absence rates often signal circulating illness before community spread becomes obvious.
- Seek Early Treatment: If you develop flu symptoms during the late-winter period, contact your healthcare provider promptly. Early antiviral treatment reduces symptom severity and duration.
Key Takeaway
The Late-Winter Flu Rebound & Influenza B happens when Influenza B rises after the early-season surge, creating a flu second wave in late winter. Because prior illness does not protect against Influenza B, many people become sick again with fever, deep cough, body aches, and extreme fatigue.
Symptoms can worsen quickly, especially in children, older adults, and those with underlying conditions. Seek emergency flu care if you develop shortness of breath, chest pain, dehydration, confusion, or symptoms that improve and then suddenly decline.
When a flu second wave hits your home, quick access to testing matters. ER of Coppell is open 24/7 with on-site rapid flu diagnostics, IV hydration, and immediate treatment without long wait.
FAQs
1. Why does flu come back in late winter?
The late-winter flu rebound happens because Influenza B peaks later than Influenza A. As precautions relax and school-aged kids return to close-contact settings, transmission accelerates through February and March.
2. How can you tell if you have Influenza A or B?
Only lab tests can confirm the strain. Rapid tests in the ER can identify Influenza B or A within 15–30 minutes to guide treatment.
3. Is Influenza B more dangerous than Influenza A?
Both can cause serious illness. Influenza B often hits children harder and may cause more stomach symptoms. Severity depends on age, health, and immunity, not the strain alone.
4. When should I go to the ER for flu symptoms?
Seek emergency flu care if you have trouble breathing, chest pain, confusion, severe dizziness, persistent vomiting, or worsening flu after initial improvement.
5. Can you get the flu twice in one season?
Yes. You can catch Influenza A and B in the same season since infection with one doesn’t protect against the other. This explains the flu second wave in late winter.